ADHD and depression may appear similar on the surface but can differ significantly in terms of underlying symptoms. While ADHD has its roots in childhood or adolescence, depressive disorders have no age restrictions – they can affect anyone at any time. Even ADD (ADHD without hyperactivity) requires treatment to address issues with focus, but feelings related to this disorder are distinct from those seen with depression.
Treatment approaches also vary depending on which condition is present; medications typically treat ADHD whereas combination therapy & antidepressants work best for depressive conditions when comorbidity occurs – meaning both illnesses exist simultaneously within a person’s life.
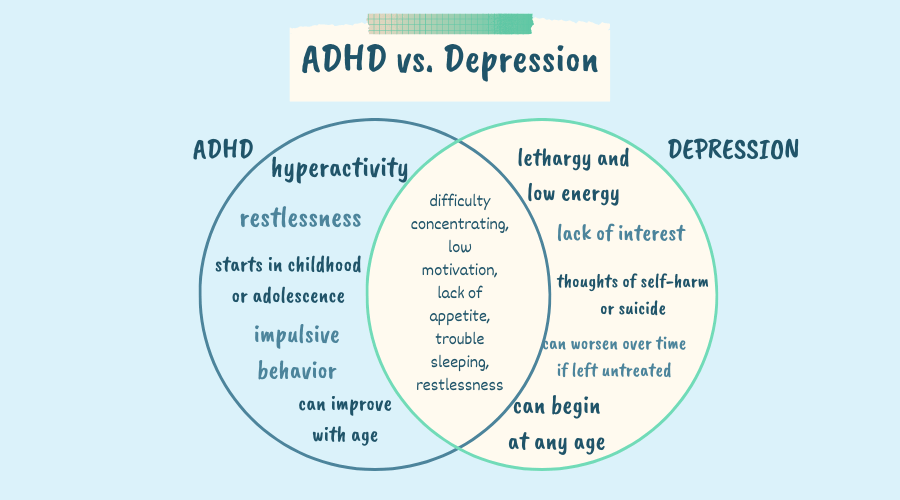
Similarities Between ADHD and Depression – Overlapping Symptoms
Both ADHD and depression can involve difficulty concentrating, low motivation, lack of appetite, trouble sleeping, and restlessness. These common symptoms can often lead to misdiagnosis.
Many people with ADHD also experience depression, making it even more difficult to distinguish between the two conditions. Besides, both conditions can lead to isolation and impaired relationships, as well as possible substance abuse. Keep reading for a detailed comparison of ADHD vs. depression.
Distinguishing ADHD vs. Depression – Key Differences
One key difference between ADHD vs. depression is that ADHD involves hyperactivity, whereas depression often includes lethargy and low energy. ADHD symptoms typically involve constant restlessness and physical activity, while depression tends to involve a lack of interest in daily activities.
In addition, ADHD often starts in childhood or adolescence, whereas depression can begin at any age. ADHD symptoms can also improve with age, while depression can worsen over time if left untreated. ADHD is also more likely to involve impulsive behavior, while depression can involve thoughts of self-harm or suicide.
Living with ADHD and depression can be devastating for the person affected, manifesting in difficulty concentrating or finding motivation as well as restlessness. Yet those same apparent symptoms mask subtle differences between these two conditions – hyperactivity vs low energy levels, age of onset, and impulse control all set them apart from one another.
What About ADD?
We mentioned hyperactivity as a key difference between ADHD vs. depression, but what about ADHD without hyperactivity, also known as ADD or ADHD-inattentive type? How does it differ from depression? Well, ADHD-inattentive type still involves problems with focus, concentration, and organization. Symptoms can overlap with depression, but the feelings are different.
For example, a person with ADD might have trouble focusing because they get distracted easily, whereas a person with depression might have trouble focusing because they lack interest in what they’re doing from the start. ADHD-inattentive type can also involve forgetfulness and easily getting sidetracked, whereas depression usually involves low self-esteem and negative thinking patterns.
Editor’s Note
If you think that you or someone close to you may be suffering from ADHD and/or depression, please contact a medical professional. Help is available, and speaking with a doctor can make all the difference.
Treating ADHD vs. Depression
The recommended treatment for ADHD vs. depression is also very different. The former is typically treated with medication for ADHD, such as stimulants or selective norepinephrine reuptake inhibitors. Therapy can also help address symptoms of ADHD and improve daily functioning.
On the other hand, symptoms of depression without ADHD are typically treated with a combination of antidepressants (such as selective serotonin reuptake inhibitors, abbreviates as SSRIs) and therapy. Antidepressants can help improve mood and alleviate symptoms, while therapy can provide coping strategies and address underlying issues.
It’s worth noting that ADHD and depression can co-occur, meaning a person may need medication and therapy to treat both conditions simultaneously. With ADHD and depression, no two situations are alike; treatment plans should always be individualized to best address the symptoms of each case. Medication and cognitive behavioral therapy can help manage these multifaceted disorders – proving that one size does not fit all!
How to Tell If You Have ADHD or Depression?
If you think you or your child may have ADHD or depression, it’s important to seek professional help. A qualified mental health provider can properly assess and diagnose these conditions, as well as recommend a treatment plan. Self-diagnosis isn’t recommended, as ADHD and depression can involve overlapping symptoms and require a trained professional to properly distinguish between the two.
See also: how to tell if someone with ADHD likes you.
Can ADHD Lead to Depression in Children and Adults?
While children and adults with ADHD can also show signs of depression, ADHD itself does not necessarily come with developing depression. However, people with ADHD can have an increased risk for other mental health issues, such as anxiety and mood disorders. ADHD can also involve challenges with academic performance, career success, and interpersonal relationships, all of which can contribute to a higher risk for depression.
Comorbid ADHD and Depression – What Does It Mean?
Comorbid conditions are when a person has more than one disorder at the same time. ADHD and depression can be comorbid to each other, meaning one can be diagnosed with ADHD and major depression simultaneously. ADHD can also be comorbid with other mental health conditions, such as anxiety or bipolar disorder.
No matter what combination of disorders an adult or child with ADHD may have, it’s important to seek professional help for proper diagnosis and treatment. Overall, there are key differences between ADHD vs. depression, but they can also co-exist and require specialized care.

Frequently Asked Questions
Can ADHD Be Mistaken for Depression?
Although difficulty concentrating, impulsivity, and difficulty managing emotions are normally associated with depression, they can sometimes be signs of ADHD. It is important to speak to a mental health professional in order to distinguish between the two conditions accurately and ensure you get proper treatment for whatever diagnosis may apply!
What Does Depression Look Like in Someone With ADHD?
Depression can manifest differently in those living with ADHD – from difficulty concentrating and feeling edgy, to struggling to regulate their emotions. Though similar symptoms are present for both people with and without this disorder, some additional expressions of depression may be seen in a person managing the condition as well.
What Is the Burnout Cycle in ADHD?
For those with ADHD, the pressures of everyday life can lead to a burnout cycle. It starts off with an overwhelming feeling that leaves them drained and unable to face tasks they normally would have no problem accomplishing. Taking on an “out-of-sight out-of mind” attitude is usually next – avoiding what needs to be done until it’s too late or guilt sets in as a reminder of all their unfinished work.
Do ADHD Meds Help With Depression?
Are you dealing with symptoms of depression? You may benefit from exploring the option of taking ADHD medications, as they have been known to improve focus and concentration which can in turn reduce feelings associated with it. However, if your situation is more severe antidepressant medication might be recommended by a doctor or mental health professional – so don’t hesitate to talk about possible options for treatment!
Can Antidepressants Help With ADHD?
For those struggling with ADHD, antidepressants can offer a much-needed reprieve. By helping to improve focus and concentration while also relieving symptoms of anxiety, restlessness, and difficulty managing emotions – they can bring significant relief from many day-to-day struggles associated with the disorder. When used in combination alongside other treatments such as lifestyle changes or therapy sessions however – it’s possible for someone to greatly manage their challenges related to ADHD more effectively than ever before.
Similar Posts: